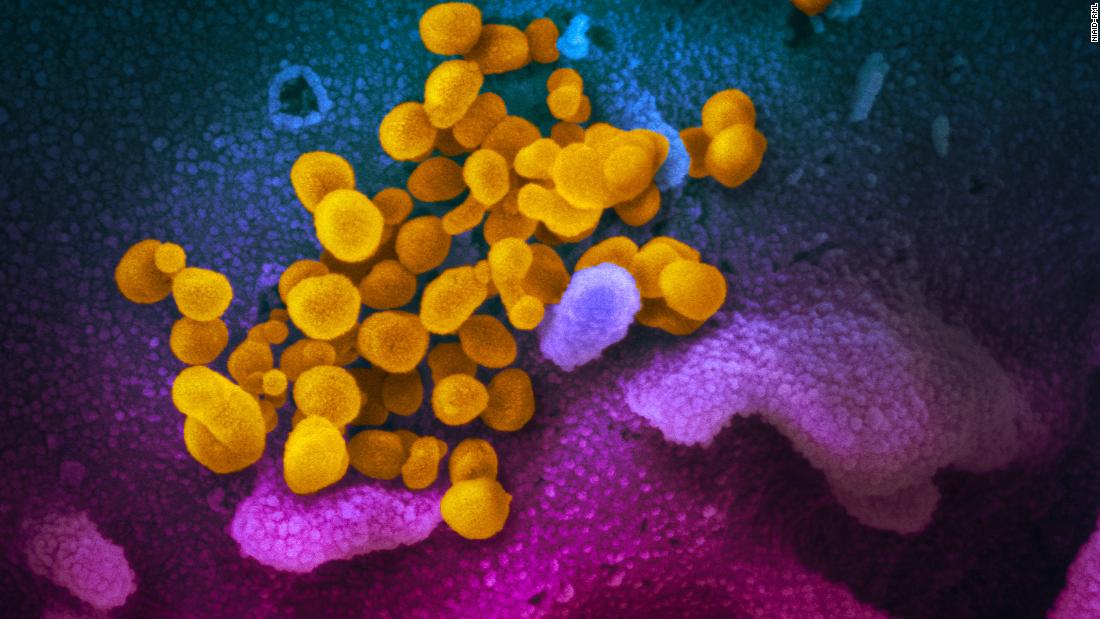
Household spread of is common and quick, CDC study finds
“Because prompt isolation of persons with COVID-19 can reduce household transmission, persons who suspect that they might have COVID-19 should isolate, stay at home, and use a separate bedroom and bathroom if feasible,” wrote a CDC-led team of researchers.
In addition, all members of the household should wear masks at all times in common spaces, the team said.
The research, part of an ongoing CDC-supported study, followed 101 people initially infected with Covid-19 in Nashville, Tennessee, and Marshfield, Wisconsin, between April and September.
Along with some 191 others who lived in their households, the infected people were trained to self-collect specimens — nasal swabs only or nasal swabs and saliva samples — each day for 14 days. In addition, each person completed a symptom diary.
Infection was quick: Over half of the people (53%) who lived with someone battling Covid-19 became infected within a week, researchers found. Some 75% of these secondary infections occurred within five days of the first symptoms in the initial patient.
“Substantial transmission occurred whether the index patient was an adult or a child,” researchers said.
A 53% household infection rate, the study said, is higher than what has been documented so far. To date, related research has reported only a 20% to 40% infection rate.
“An important finding of this study is that fewer than one half of household members with confirmed SARS-CoV-2 infections reported symptoms at the time infection was first detected,” the study authors wrote.
“Many reported no symptoms throughout 7 days of follow-up, underscoring the potential for transmission from asymptomatic secondary contacts and the importance of quarantine.”
Isolate yourself or your loved one
Staying isolated from other household members can be challenging, especially if you are in a small space or there are children in the home.
“If it’s a child that you have to care for, then you may have to make the decision to isolate one adult with the child,” she added. “That adult would be caring for the child, and the other adult would be responsible for the rest of family.”
“Know who your neighbors are, even what your neighborhood social network might be,” said Radesky, an assistant professor of pediatrics at the University of Michigan. “You may not be that close interpersonally, but someone may be willing to do a grocery store drop-off, or pick-up medications because we’re all in this together.”
The rest of the family should practice isolation as well, Radesky added.
“Unfortunately you need to keep the whole household under isolation,” she said. “The patterns of Covid-19 spread suggest that clusters of people who live close together are at highest risk of getting it from one another. If children are part of that household, they may show minimal symptoms but still be contagious.”
If you live alone, your challenge is to monitor your symptoms and care for yourself when you’re not feeling well. Be sure to have a plan in place to get food and medications delivered to your home, and find someone who can be responsible for virtually checking in on you on a regular basis.
Stock or ask loved ones to provide the room with all relevant forms of entertainment: TV, computer, iPad, books, even games that you could play via FaceTime or Skype.
A supply checklist
Don’t hesitate to order online or ask loved ones to provide basic supplies:
- A working thermometer to monitor fever, which is considered to be 100 degrees Fahrenheit (37.7 degrees Celsius), and a method to clean it, such as isopropyl alcohol
- Fever-reducing medications, such as acetaminophen
- A box of rubber or latex disposable gloves and face masks
- A 60- or 90-day supply of necessary prescription medicines
- Regular soap and 70% alcohol-based hand sanitizer (antibacterial soap isn’t necessary if you wash properly, and that way you won’t contribute to the world’s growing antibiotic-resistant superbugs)
- Tissues to cover sneezes and coughs. But there is really no need to hoard toilet paper — this is a respiratory disease
- Regular cleaning supplies, kitchen cleaning gloves and trash can liners
- Disinfectant cleaning supplies — the CDC suggests picking from a list that meets the virus-fighting standards of the US Environmental Protection Agency, but says you can also make your own version by using 1/3 cup unexpired bleach per gallon of water or 4 teaspoons bleach per quart of water. Never mix bleach with ammonia or any other cleanser — it produces toxic gases
Cover up and disinfect
If you’re sick, the CDC says to use a face mask around other people, such as when going to the doctor or hospital.
Maximize isolation and protective actions, Altmann stressed.
“You can have a healthy person leave the sick one food and drinks at the door, and then go wash their hands,” Altmann explained. “Wear gloves to pick up the empty plates, take them back to the kitchen and wash them in hot water with soap, or preferably with a dishwasher, and wash your hands again.”
Do not share drinking glasses, cups, forks or other eating utensils or dishes, the CDC says. Don’t share towels or bedding with other people in your home. When doing laundry, don’t shake the sick person’s dirty clothes to “minimize the possibility of dispersing virus through the air.”
And caregivers should wear disposable gloves when handling that dirty laundry, the CDC says, throwing them away after each use.
“If using reusable gloves, those gloves should be dedicated for cleaning and disinfection of surfaces for Covid-19 and should not be used for other household purposes. Clean hands immediately after gloves are removed,” the CDC advises.
Dedicate a lined trash can for any tissues or other paper or disposable products used by a sick person, the CDC says, adding that caregivers should “use gloves when removing garbage bags, handling and disposing of trash. Wash hands after handling or disposing of trash.”
And remember: Call 911 immediately if you or your loved ones have any of these symptoms: increased or sudden difficulty breathing or shortness of breath; a persistent pain or pressure in the chest; and any sign of oxygen deprivation, such as new confusion, bluish lips or face, or you can’t arouse the sick person.
While these are key danger signs, this is not an exhaustive list, said American Medical Association President Dr. Patrice Harris, so call if anything concerns you.
“If the symptoms don’t get better or they worsen you should call your health care provider, the urgent care or the emergency department,” Harris said. “And if the shortness of breath is severe, immediately call 911.”
Keeping everyone else from getting sick
To be clear: After a positive Covid-19 diagnosis, everyone in the house needs to isolate themselves from the outside world as much as possible.
“I would recommend that families find friends who can drop off essential groceries or medications, not go to work, and not play with other children — even outside,” Radesky said.
“If you don’t have friends who can drop off groceries or essential items, see if the local stores can deliver the items for you — I’m sure they would appreciate not having a potential Covid-19 exposure in their store,” she added.
If a family member without symptoms believes it is absolutely essential to go outside to the grocery store, pharmacy or to check on a family member, be aware that you may well be contagious and anything you touch could transfer the virus — even without symptoms.
“I would urge people not to do this,” Radesky said. “The way we will beat this virus is by reducing the number of times that each infected person transmits the virus to another person. So the more you can do to stop the virus in its tracks — in other words, your family doesn’t give it to anyone else, and you don’t bring it to your workplace or a local store — the sooner we will be done with this!”
To reduce virus transfer inside your home, try to keep an air flow in the rest of the home with opened windows or doors with screens, if weather permits. You can also add air filtering devices to your home.
“Improving ventilation helps remove respiratory droplets from the air,” the CDC says.
Have everyone wash their hands at every opportunity. Clean and disinfect all those commonly shared surfaces — don’t forget the refrigerator and microwave handles!
Keep everyone as stress-free as possible — a hard task for sure — and focus on healthy eating, regular exercise and quality sleep.
Even though there is no indication that pets can give or get Covid-19, the CDC suggests keeping pets away from sick people.
“Since animals can spread other diseases to people, it’s always a good idea to practice healthy habits around pets and other animals,” the CDC says. “If you must care for your pet or be around animals while you are sick, wash your hands before and after you interact with pets.”
When is your home isolation over?
For those with symptoms, the CDC says you can be around others when:
- It’s been 10 days or more since symptoms first appeared
- AND you’ve gone 24 hours with no fever without the use of fever-reducing medications
- AND other symptoms of COVID-19 are improving
“A limited number of persons with severe illness may produce replication-competent virus beyond 10 days that may warrant extending duration of isolation and precautions for up to 20 days after symptom onset,” the CDC says. Consider consultation with infection control experts, the agency says.
A loss of taste and smell can remain for weeks or even months after recovery, the CDC notes, but that does not mean you need to remain isolated.
However, if you have a severely weakened immune system or were more severely sick with Covid-19 — such as being admitted to a hospital and needing oxygen — the rules change, according to the CDC:
“Your healthcare provider may recommend that you stay in isolation for longer than 10 days after your symptoms first appeared (possibly up to 20 days),” the CDC says.
“Persons who are severely immunocompromised may require testing to determine when they can be around others. Talk to your healthcare provider for more information.”
These are scary times, but hopefully these tips will help ease your anxiety and prepare you and your family for the worst, while hoping and striving for the best.
![]()